Experiencing a delayed ovulation can be a source of confusion and concern, especially when trying to conceive or simply understanding your body's rhythm. Late ovulation, defined as ovulation occurring significantly later than the typical mid-cycle (Day 14-16 in a 28-day cycle), arises from various underlying factors, most commonly hormonal imbalances, Polycystic Ovary Syndrome (PCOS), and significant lifestyle influences like stress or drastic weight changes. Understanding what causes late ovulation is crucial for managing fertility and addressing potential health issues.
Key Takeaways
- Late ovulation is generally defined as occurring after day 21 of a menstrual cycle, or significantly later than expected based on individual cycle length.
- Hormonal imbalances, particularly disruptions in follicle-stimulating hormone (FSH) and luteinizing hormone (LH), are primary drivers.
- Polycystic Ovary Syndrome (PCOS) is one of the most common medical conditions causing late or irregular ovulation.
- Significant lifestyle factors like chronic stress, extreme exercise, poor nutrition, and substantial weight fluctuations can all delay ovulation.
- Underlying medical conditions such as thyroid disorders, hyperprolactinemia, and perimenopause can also contribute to delayed ovulation.
- Tracking ovulation through methods like Basal Body Temperature (BBT) and Ovulation Predictor Kits (OPKs) is key to identifying late ovulation.
- Consulting a healthcare provider is essential for proper diagnosis and personalized treatment plans if late ovulation is a persistent concern, especially when trying to conceive.
Quick Answer
Late ovulation is primarily caused by hormonal disruptions that interfere with the normal development and release of an egg from the ovary. Common culprits include conditions like Polycystic Ovary Syndrome (PCOS), significant physical or emotional stress, substantial weight fluctuations, and underlying thyroid imbalances, all of which can alter the delicate timing of the menstrual cycle.
What Are the Hormonal Imbalances That Cause Late Ovulation?
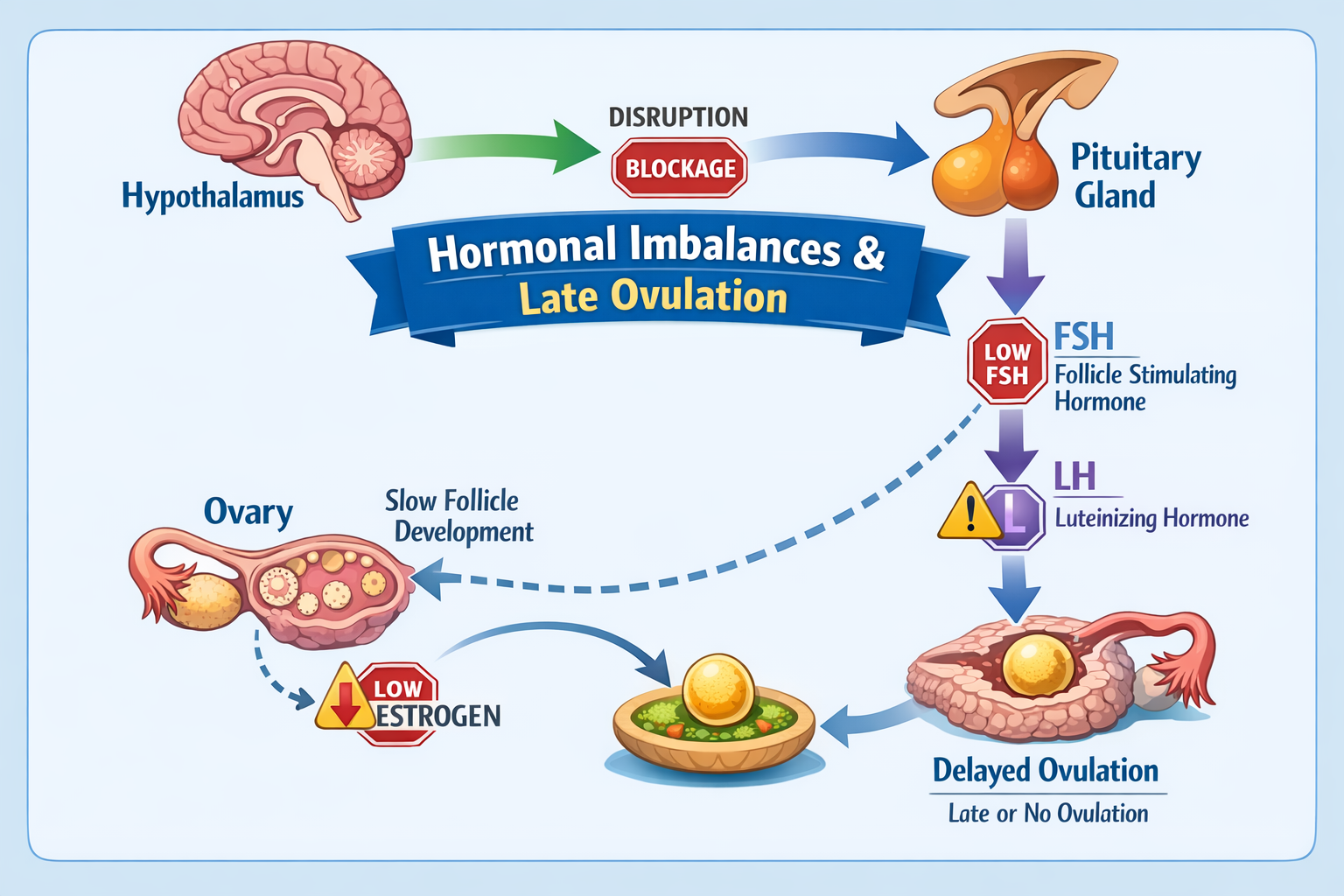
Hormonal imbalances are a leading cause of late ovulation because the entire menstrual cycle is orchestrated by a complex interplay of hormones. When these hormones are out of sync, the follicular development and egg release can be significantly delayed or disrupted.
The process of ovulation depends on a precise sequence and surge of several key hormones:
- Follicle-Stimulating Hormone (FSH): Produced by the pituitary gland, FSH stimulates the growth of ovarian follicles in the first half of the cycle (follicular phase). Insufficient FSH can lead to slow or incomplete follicle development, pushing back the ovulation date.
- Luteinizing Hormone (LH): Also from the pituitary, a surge in LH triggers the final maturation and rupture of the dominant follicle, releasing the egg. If the LH surge is delayed, weak, or absent, ovulation will not occur on time.
- Estrogen: As follicles grow, they produce estrogen. Rising estrogen levels signal the pituitary to prepare for the LH surge. Low estrogen production can delay this signal, consequently delaying LH and ovulation.
- Progesterone: While primarily active after ovulation, imbalances in progesterone from previous cycles can subtly affect the next cycle's timing.
- Androgens: Elevated levels of androgens (male hormones) can interfere with follicular development and contribute to ovulatory dysfunction, often seen in conditions like PCOS.
How Hormonal Imbalances Impact Ovulation:
- Delayed Follicle Growth: If FSH levels are suboptimal, follicles may grow slowly, taking longer to reach the size needed for ovulation.
- Absent or Weak LH Surge: A critical component of ovulation is the LH surge. If it doesn't happen, or is too weak, the egg won't be released. Conditions like PCOS often involve issues with LH regulation.
- Anovulation: In some cases, hormonal imbalances can lead to anovulation, where ovulation doesn't occur at all within a cycle. This often manifests as very late or missed periods.
If you suspect hormonal imbalances are affecting your cycle, a healthcare provider can conduct blood tests to measure your hormone levels. This is particularly important if you're experiencing consistently irregular cycles or struggling to conceive. Utilizing tools like an AI Ovulation Predictor can help identify patterns in your cycle, which you can then discuss with your doctor.
How Do Medical Conditions Contribute to Delayed Ovulation?

Certain medical conditions directly impact the endocrine system, leading to hormonal imbalances that cause late ovulation or even anovulation. Recognizing these conditions is a critical step in diagnosis and treatment.
Polycystic Ovary Syndrome (PCOS)
PCOS is arguably the most common endocrine disorder among women of reproductive age and a primary cause of late or irregular ovulation. In PCOS, the ovaries may contain multiple small follicles (cysts) that don't mature properly. The hormonal profile of PCOS often includes:
- Elevated Androgens: Higher levels of male hormones interfere with the normal follicular development and egg release.
- Insulin Resistance: Many women with PCOS have insulin resistance, which can lead to higher insulin levels. High insulin can stimulate the ovaries to produce more androgens, exacerbating ovulatory dysfunction.
- Imbalanced LH to FSH Ratio: Women with PCOS often have chronically elevated LH levels and relatively lower FSH, preventing a clear LH surge and hindering follicle maturation.
Because of these hormonal disruptions, ovulation in women with PCOS can be infrequent, unpredictable, or absent entirely.
Thyroid Disorders
Both an underactive thyroid (hypothyroidism) and an overactive thyroid (hyperthyroidism) can significantly affect the menstrual cycle and fertility.
- Hypothyroidism: Low levels of thyroid hormones can interfere with the metabolism of estrogen, leading to irregular cycles, including late ovulation. It can also increase prolactin levels, which can suppress ovulation.
- Hyperthyroidism: High levels of thyroid hormones can also disrupt the delicate hormonal balance required for regular ovulation.
Hyperprolactinemia
This condition involves abnormally high levels of prolactin, the hormone responsible for milk production. Elevated prolactin, even outside of pregnancy or breastfeeding, can inhibit the release of GnRH (Gonadotropin-Releasing Hormone) from the hypothalamus, which in turn suppresses FSH and LH production, leading to delayed or absent ovulation.
Perimenopause
As women approach menopause, ovarian function naturally begins to decline. This transition, known as perimenopause, often involves erratic hormone levels, leading to irregular cycles and delayed or skipped ovulations as the body's egg supply diminishes.
If you're experiencing very late or absent periods, especially with other symptoms like unexplained weight changes, fatigue, or excessive hair growth, it's essential to consult a doctor. They can perform diagnostic tests to identify any underlying medical conditions.
What Lifestyle Factors Affect Ovulation Timing?
Our daily habits and environment play a significant role in the delicate hormonal balance that regulates ovulation. Various lifestyle factors can directly interfere with this balance, leading to late ovulation.
Stress
Chronic physical or psychological stress can significantly disrupt the hypothalamic-pituitary-ovarian (HPO) axis, the central command center for reproductive hormones.
- Cortisol Release: When stressed, the body releases cortisol. High cortisol levels can suppress GnRH, thereby reducing FSH and LH, which are essential for follicle development and ovulation.
- Delayed Ovulation: This suppression can directly delay or even temporarily halt ovulation. Intense emotional stress, major life changes, or even overtraining can trigger this response.
Managing stress through techniques like mindfulness, yoga, adequate sleep, and seeking support can help regulate the HPO axis.
Weight Fluctuations (Underweight or Overweight)
Maintaining a healthy Body Mass Index (BMI) is crucial for regular ovulation.
- Being Underweight: Very low body fat can signal to the body that it's not a safe environment for pregnancy. The body may conserve energy by suppressing reproductive hormones, leading to anovulation or significantly delayed ovulation. This is common in athletes with very low body fat or individuals with eating disorders.
- Being Overweight/Obese: Excess body fat, particularly around the abdomen, can lead to increased estrogen production (fat cells convert androgens into estrogen) and insulin resistance. Both can disrupt the HPO axis, interfere with follicular development, and contribute to late ovulation, often mimicking aspects of PCOS.
A balanced diet and moderate, regular exercise are key to maintaining a healthy weight and supporting regular ovulation.
Excessive Exercise
While regular physical activity is beneficial, extreme or prolonged high-intensity exercise, especially when combined with insufficient caloric intake, can mimic the effects of being underweight. This can lead to:
- Functional Hypothalamic Amenorrhea (FHA): A condition where the hypothalamus slows or stops releasing GnRH, resulting in low FSH and LH, and consequently, delayed or absent ovulation.
- Delayed Puberty/Ovulation: This is often seen in professional athletes or individuals with rigorous training regimens.
Finding a balance in your exercise routine is important for supporting reproductive health.
Diet and Nutrition
What we eat can influence hormone production and sensitivity.
- Nutrient Deficiencies: Deficiencies in essential vitamins and minerals (e.g., Vitamin D, B vitamins, iron) can impact overall health and indirectly affect hormonal balance.
- Blood Sugar Regulation: Diets high in refined carbohydrates and sugars can contribute to insulin resistance, particularly in predisposed individuals, which can exacerbate ovulatory dysfunction seen in PCOS.
- Caffeine and Alcohol: While moderate intake is generally safe, excessive consumption of caffeine and alcohol may negatively impact fertility and hormonal balance, although direct links to late ovulation are still being researched.
Prioritizing a balanced diet rich in whole foods, lean proteins, and healthy fats supports overall endocrine function.
Understanding these lifestyle influences can empower you to make changes that promote healthier, more predictable menstrual cycles. Tracking your cycle with a tool like a Cycle Length Calculator can help you identify patterns and link them to your lifestyle choices.
How Is Late Ovulation Diagnosed and Managed?

Diagnosing late ovulation involves a combination of tracking, medical history, and specific diagnostic tests. Effective management typically addresses the underlying cause to help regulate the menstrual cycle.
Diagnosis
-
Cycle Tracking: The first step is diligent cycle tracking. This includes:
- Basal Body Temperature (BBT) Charting: Taking your temperature every morning can reveal a temperature shift after ovulation. A sustained higher temperature indicates ovulation has occurred. A delayed rise suggests late ovulation. Our BBT Chart Tool can assist with this.
- Ovulation Predictor Kits (OPKs): OPKs detect the LH surge, which typically happens 24-36 hours before ovulation. If your LH surge consistently appears later than cycle day 14-16 (or later than typical for your cycle length), it indicates late ovulation. For clarity on typical cycles, an Ovulation Symptoms Checker can be useful.
- Cervical Mucus Monitoring: Changes in cervical mucus consistency (becoming clear, stretchy, and egg-white-like) indicate increasing estrogen and approaching ovulation. A delayed appearance of this fertile mucus suggests late ovulation.
- Menstrual Cycle Calendar: Simply noting the start and end dates of your period can highlight irregularities.
-
Medical History and Physical Exam: Your doctor will ask about your menstrual history, symptoms (e.g., irregular periods, acne, hair growth, weight changes), lifestyle, and any family history of conditions like PCOS or thyroid issues. A physical exam may include checking for signs of hormonal imbalances.
-
Blood Tests:
- Hormone Levels: Blood tests can measure levels of FSH, LH, estrogen, prolactin, thyroid-stimulating hormone (TSH), and androgens to identify specific imbalances.
- Glucose and Insulin: For suspected PCOS, tests for insulin resistance might be conducted.
-
Ultrasound: A transvaginal ultrasound can assess ovarian health, check for the presence of follicles, and look for characteristics of PCOS (e.g., multiple small cysts on the ovaries).
Management and Treatment
The approach to managing late ovulation depends entirely on the identified cause.
| Cause of Late Ovulation | Management Strategies |
|---|---|
| PCOS | Lifestyle modifications (diet, exercise for weight management), insulin-sensitizing medications (e.g., Metformin), ovulation-inducing medications (e.g., Clomiphene Citrate, Letrozole). |
| Thyroid Disorders | Medication to balance thyroid hormone levels (e.g., levothyroxine for hypothyroidism). Regular monitoring of TSH levels. |
| Hyperprolactinemia | Medications to lower prolactin levels (e.g., bromocriptine, cabergoline). |
| Stress | Stress management techniques (meditation, yoga, therapy), adequate sleep, setting boundaries, addressing underlying stressors. |
| Weight Imbalances (Under/Overweight) | Nutritional counseling, healthy eating plans, regular moderate exercise to achieve and maintain a healthy BMI. Avoid extreme dieting or excessive exercise. |
| Perimenopause | While ovulation can become naturally erratic, management focuses on symptom relief and potentially fertility treatments if conception is desired and feasible. |
| Unexplained Late Ovulation | Continued cycle tracking, lifestyle optimization, and sometimes empirical use of ovulation-inducing medications under medical supervision. |
For those trying to conceive, understanding and managing late ovulation is critical, as it directly impacts the fertile window. Our Late Ovulation Calculator – Adjusted Fertile Window & Implantation Dates can help predict your fertile window based on adjusted ovulation dates. Always consult with a healthcare professional to determine the best course of action for your specific situation.
Conclusion
Understanding what causes late ovulation is the first step towards better reproductive health and family planning. Whether it stems from common conditions like PCOS, hormonal imbalances, or lifestyle factors such as stress and significant weight changes, identifying the root cause is paramount. Consistent cycle tracking using methods like BBT and OPKs can provide valuable insights, but a healthcare provider's expertise is essential for accurate diagnosis and a personalized management plan. By addressing these underlying issues, many women can achieve more regular cycles and optimize their chances of conception. If you're consistently experiencing late ovulation or have concerns about your fertility, don't hesitate to seek professional medical advice.
Related Reading
- Late Ovulation: Chances, Timing, & Implantation Success
- Fertile Window Calculator | Find Your 6-Day Conception Window
- Implantation Date Calculator – Estimate Implantation Timing Accurately
FAQ
Q1: What day is considered late ovulation?
A1: While a typical cycle has ovulation around day 14, ovulation occurring consistently after day 21, or significantly later than your individual cycle's expected mid-point, is generally considered late ovulation.
Q2: Can you still get pregnant if you ovulate late?
A2: Yes, you can still get pregnant if you ovulate late. The key is to identify your fertile window based on your actual ovulation date, not just cycle day 14. Pregnancy chances might be slightly lower per cycle, but conception is certainly possible.
Q3: How do I know if I'm ovulating late?
A3: You can determine late ovulation by consistent tracking methods such as Basal Body Temperature (BBT) charting, using Ovulation Predictor Kits (OPKs) that detect the LH surge, and observing changes in your cervical mucus.
Q4: Can stress cause late ovulation?
A4: Yes, chronic or significant stress can cause late ovulation. Stress hormones like cortisol can interfere with the signals from the brain that regulate the menstrual cycle, delaying or even preventing ovulation.
Q5: What is the most common cause of late ovulation?
A5: Polycystic Ovary Syndrome (PCOS) is one of the most common medical conditions causing late or irregular ovulation due to its impact on hormonal balance. Lifestyle factors like stress and weight imbalances are also very common contributors.
Q6: Does late ovulation affect implantation?
A6: Late ovulation itself does not directly affect implantation, but it can shift the implantation window. If ovulation occurs later, then the typical implantation window (6-12 days post-ovulation) will also be delayed accordingly.
Q7: Can late ovulation be a sign of perimenopause?
A7: Yes, as women approach perimenopause, hormonal fluctuations and declining ovarian reserve can lead to irregular cycles, including late or anovulatory cycles, before menstruation ceases entirely.
Q8: Should I see a doctor if I ovulate late?
A8: If you are consistently experiencing late ovulation, especially if you are trying to conceive, have other concerning symptoms (like excessive hair growth, severe acne, or unexplained weight changes), or if your cycles are very irregular, it is advisable to consult a doctor.
