The journey to parenthood is deeply personal, and for many women, the question, "What are my chances of getting pregnant at 40?" becomes a central focus as they approach or enter their fifth decade. While it's true that fertility naturally declines with age, becoming pregnant at 40 is absolutely possible for many individuals, though it often requires more awareness, patience, and sometimes, medical intervention. This comprehensive guide will explore the biological realities, available options, and practical steps to help you understand your unique prospects in 2026.
Key Takeaways
- Natural conception rates decline significantly after age 35; at 40, the chance per menstrual cycle is generally around 5%.
- Egg quality and quantity decrease with age, increasing risks of miscarriage and genetic abnormalities.
- Fertility treatments like IVF can significantly improve conception odds for women over 40, with success rates varying based on individual factors.
- Lifestyle choices, including diet, exercise, and stress management, play a crucial role in optimizing fertility at this age.
- Consulting with a fertility specialist early on is highly recommended to assess ovarian reserve and discuss personalized strategies.
- Understanding your fertile window through ovulation tracking is essential for maximizing natural conception attempts.
- Pregnancy over 40 carries increased risks for both mother and baby, requiring close medical supervision.
- Donor eggs present a viable and often highly successful option for women facing challenges with their own egg quality.
Quick Answer
For women aged 40, the chance of natural conception in any given menstrual cycle is generally estimated to be around 5%, decreasing from approximately 20% in their late 20s and early 30s. While pregnancy is still possible, the biological decline in egg quantity and quality means that conception may take longer, and the likelihood of needing assisted reproductive technologies (ART) like IVF increases significantly.
How Does Age Impact a Woman's Fertility at 40?
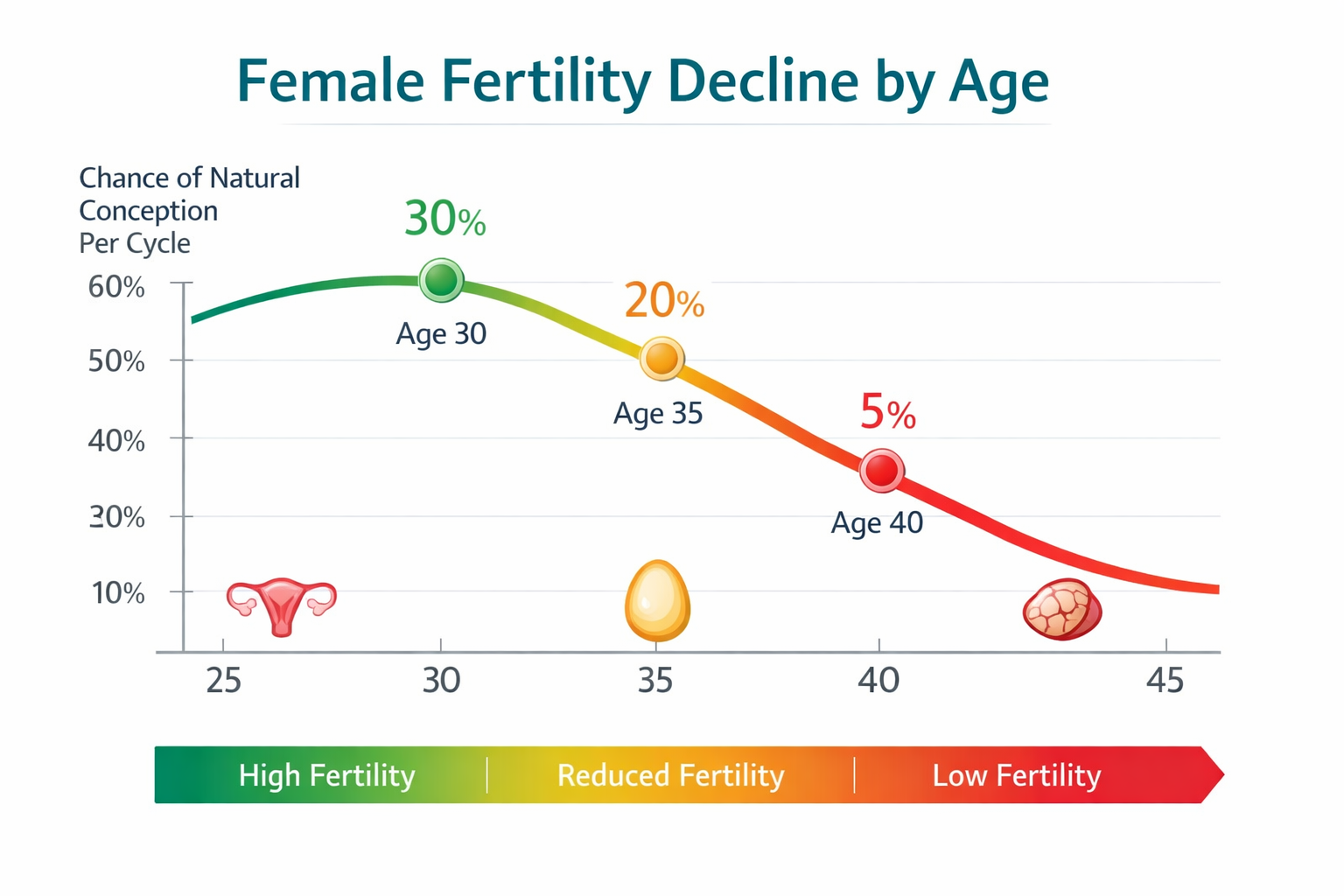
At age 40, a woman's fertility is markedly different from her younger years due to a natural, progressive decline in both the quantity and quality of her eggs. This biological reality means that while some women conceive naturally, the overall odds are significantly lower compared to women in their 20s or early 30s.
Specifically, women are born with all the eggs they will ever have, and this reserve diminishes over time. By age 40, the remaining eggs are fewer in number, and a higher percentage of them are likely to have chromosomal abnormalities, which can lead to a reduced chance of conception, increased risk of miscarriage, and a higher likelihood of genetic conditions in a baby. The decline in ovarian reserve also impacts hormonal regularity, potentially leading to shorter fertile windows or anovulatory cycles (cycles where no egg is released). For more detailed statistics on age-related fertility, consider using a Pregnancy Chance by Age Calculator.
Understanding Ovarian Reserve
Ovarian reserve refers to the number and quality of eggs remaining in a woman's ovaries. Several tests can help assess this:
- Anti-Müllerian Hormone (AMH) Test: This blood test measures the level of AMH, a hormone produced by cells in ovarian follicles. Higher AMH levels generally indicate a larger ovarian reserve.
- Follicle-Stimulating Hormone (FSH) Test: High FSH levels, typically tested on day 3 of the menstrual cycle, can indicate that the ovaries are working harder to stimulate egg growth, suggesting a diminished ovarian reserve.
- Antral Follicle Count (AFC): An ultrasound procedure that counts the number of small follicles in the ovaries, providing an estimate of the remaining egg supply.
These tests help fertility specialists understand an individual's unique biological picture, offering a more personalized answer to "What are my chances of getting pregnant at 40?" based on their current ovarian health. For example, a woman with surprisingly good AMH and FSH levels for her age might have better natural odds than average, while someone with significantly diminished reserve might be advised to consider assisted reproductive options sooner.
What Are My Chances of Getting Pregnant at 40 Naturally?

Your chances of getting pregnant naturally at 40 are significantly lower than in your younger years, with estimates generally placing the per-cycle probability at around 5%. This means that for every 100 women aged 40 trying to conceive naturally in a given month, approximately 5 will succeed.
While 5% may seem low, it's crucial to remember that this is a per-cycle average, and individual experiences vary widely. Some women will conceive quickly, while others may take longer or require assistance. The cumulative chance of conceiving within 12 months for a 40-year-old woman attempting natural conception is approximately 20%. This decrease in natural fertility is primarily due to the decline in both the quantity and quality of eggs, which makes it harder to conceive and increases the risk of early pregnancy loss. To get a quick estimate of your monthly odds, you can use a Pregnancy Probability Calculator.
Factors Influencing Natural Conception at 40
Several factors beyond age can impact natural conception odds:
- Overall Health: Good general health, including a healthy weight, balanced diet, and absence of chronic conditions (like uncontrolled diabetes or thyroid issues), can support fertility.
- Male Partner's Fertility: The age and health of the male partner also play a role, as male fertility can decline with age, affecting sperm quality and count.
- Previous Pregnancies: Women who have conceived naturally before may have slightly better odds than those who haven't.
- Menstrual Cycle Regularity: Regular cycles generally indicate more consistent ovulation, which is essential for natural conception. An irregular cycle may indicate an underlying issue that needs addressing.
- Lifestyle Choices: Avoiding smoking, excessive alcohol, and maintaining a healthy Body Mass Index (BMI) are critical for optimizing natural fertility.
When to Seek Medical Advice for Natural Conception
If you are 40 or older and have been trying to conceive naturally for six months without success, it is strongly recommended to consult a fertility specialist. This timeframe is shorter than for younger women (typically 12 months for those under 35) because age significantly impacts fertility, and prompt evaluation can help identify any underlying issues and explore effective treatment options. Early consultation is key to maximizing your chances.
What Are My Chances of Getting Pregnant at 40 with Fertility Treatments?
With fertility treatments, your chances of getting pregnant at 40 can significantly increase compared to natural attempts, although success rates vary widely based on the specific treatment, individual health factors, and the source of eggs. For women over 40, In Vitro Fertilization (IVF) is often the most recommended and effective treatment.
Using a woman's own eggs, the live birth rate per IVF cycle for women aged 40-42 is typically around 10-15%, according to data from organizations like the Society for Assisted Reproductive Technology (SART). This rate tends to decrease further with each successive year. However, if using donor eggs, the success rates for women over 40 can be much higher, often reaching 40-50% or more per cycle, as the egg quality is typically from a younger, fertile donor. Therefore, choosing the right treatment strategy is crucial and often involves a personalized consultation with a fertility expert.
Common Fertility Treatments and Their Effectiveness at 40
| Treatment Option | Description | Estimated Live Birth Rate per Cycle (Age 40-42, Own Eggs) | Considerations at Age 40 |
|---|---|---|---|
| Ovulation Induction (OI) | Medications (e.g., Clomid, Letrozole) used to stimulate egg release in women with irregular or absent ovulation. Often combined with timed intercourse. | Low (typically <5%), mainly effective if primary issue is ovulation dysfunction. | Less effective if the primary issue is diminished egg quality/quantity. May be considered as a first step if ovulation is the only concern. |
| Intrauterine Insemination (IUI) | Sperm is collected, washed, and then directly inserted into the uterus around the time of ovulation. Often combined with ovulation induction. | Low (typically 5-10%), often similar to natural conception rates if male factor is not the primary issue. | Limited success if egg quality/quantity is the main barrier. Multiple cycles may be needed. |
| In Vitro Fertilization (IVF) | Eggs are retrieved from the ovaries, fertilized with sperm in a lab, and the resulting embryo(s) are transferred into the uterus. Can use own eggs or donor eggs. | 10-15% (own eggs); 40-50%+ (donor eggs) | Most effective option for women over 40. Success rates with own eggs decrease significantly with age, emphasizing the benefit of donor eggs for some. Requires significant financial and emotional investment. |
| Donor Egg IVF | IVF using eggs from a younger donor, fertilized with partner's sperm (or donor sperm), then transferred into the recipient's uterus. | High (40-50%+), largely dependent on donor's age and health. | Highly successful due to superior egg quality. Bypasses age-related egg quality issues. Can be emotionally complex and financially demanding. |
| Embryo Freezing (Egg Freezing) | While not a treatment for current conception, freezing eggs or embryos at a younger age (e.g., in your 30s) significantly improves future IVF success rates, as it preserves younger, healthier eggs/embryos. | If eggs/embryos were frozen before age 35-38, success rates at 40+ can mirror those of the age at which they were frozen (e.g., 20-30%+ per transfer cycle). | Not an option for immediate conception at 40 unless eggs/embryos were previously frozen. Serves as a proactive measure. |
When considering IVF, the number of cycles attempted also plays a role. While the per-cycle rate is modest, the cumulative chance of success after 2-3 cycles can be higher. However, each cycle is a significant undertaking, both physically and emotionally.
What Are the Risks of Pregnancy at 40?

Pregnancy at 40, while increasingly common, carries a higher risk of complications for both the mother and the baby compared to pregnancies in younger women. These risks necessitate closer medical monitoring and specialized care throughout gestation.
Maternal risks include a higher incidence of gestational diabetes, high blood pressure (preeclampsia), placental problems (such as placenta previa or placental abruption), and an increased likelihood of requiring a Cesarean section. For the baby, there's a greater risk of chromosomal abnormalities like Down syndrome, premature birth, low birth weight, and stillbirth. The risk of miscarriage also increases significantly with maternal age, reaching approximately 40% at age 40 (American College of Obstetricians and Gynecologists, 2023).
Common Risks and How They Are Managed
- Gestational Diabetes: Higher risk due to age-related changes in metabolism. Managed with dietary modifications, exercise, and sometimes medication (insulin). Regular screening is vital.
- Preeclampsia: Increased risk of high blood pressure and organ damage. Closely monitored with regular blood pressure checks and urine tests for protein. Early detection and management are key.
- Chromosomal Abnormalities: The risk of conditions like Down syndrome significantly increases. Screening tests (e.g., NIPT, first-trimester screening) and diagnostic tests (e.g., amniocentesis, CVS) are offered to assess risk.
- Miscarriage: As mentioned, the risk is higher due to egg quality. While often unavoidable, early and regular prenatal care helps monitor the pregnancy.
- Preterm Birth/Low Birth Weight: Increased surveillance for early labor signs and interventions to prolong pregnancy if necessary.
- Cesarean Section: Higher rates of C-sections, often due to labor complications, pre-existing conditions, or fetal distress. Birth plans are discussed in detail with the medical team.
It's important to have an open and honest discussion with your healthcare provider about these risks and how they will be monitored and managed throughout your pregnancy. A strong support system, including a knowledgeable medical team, is invaluable for navigating a pregnancy at 40.
How Can I Improve My Chances of Getting Pregnant at 40?
Improving your chances of getting pregnant at 40 involves a multi-faceted approach, combining proactive health measures, informed lifestyle choices, and strategic fertility tracking. While age is a fixed factor, optimizing other controllable elements can significantly enhance your prospects of conception.
Focusing on a balanced diet, regular moderate exercise, stress reduction, and avoiding detrimental habits like smoking and excessive alcohol consumption are crucial. Additionally, understanding your menstrual cycle deeply and accurately identifying your fertile window through tracking methods can maximize the effectiveness of natural attempts. For example, using tools like an Ovulation Symptoms Checker or a Fertile Window Calculator can pinpoint your most fertile days.
Actionable Steps to Boost Fertility
-
Prioritize a Nutrient-Rich Diet:
- Focus on whole foods: Emphasize fruits, vegetables, lean proteins, and whole grains.
- Include fertility-boosting nutrients: Folate, omega-3 fatty acids, antioxidants (found in berries, nuts, dark leafy greens), and iron are particularly important.
- Limit processed foods, sugar, and unhealthy fats: These can contribute to inflammation and hormonal imbalances.
-
Maintain a Healthy Weight:
- Being underweight or overweight can disrupt hormonal balance and ovulation.
- Aim for a healthy Body Mass Index (BMI) through a combination of diet and exercise.
-
Engage in Moderate Exercise:
- Regular physical activity improves overall health, reduces stress, and can positively impact hormone levels.
- Avoid excessive, high-intensity exercise, which can sometimes negatively affect ovulation. Aim for activities like walking, swimming, or yoga.
-
Manage Stress Effectively:
- Chronic stress can impact hormone regulation.
- Incorporate stress-reducing techniques such as meditation, yoga, deep breathing exercises, or spending time in nature.
-
Avoid Harmful Substances:
- Quit smoking: Smoking significantly impairs egg quality and accelerates ovarian aging.
- Limit alcohol and caffeine: Reduce or eliminate alcohol intake, and moderate caffeine consumption.
- Avoid illicit drugs: These can have severe negative impacts on fertility and pregnancy.
-
Track Your Cycle and Ovulation:
- Understanding your menstrual cycle and identifying your fertile window is paramount.
- Use ovulation predictor kits (OPKs), basal body temperature (BBT) tracking, and monitor cervical mucus. An Easy Ovulation Calculator can help predict your fertile days.
- Time intercourse strategically during your most fertile days.
-
Consult a Fertility Specialist Early:
- Given the age factor, it's wise to consult a specialist after 6 months of trying to conceive, or even sooner if you have known fertility concerns.
- They can conduct tests (e.g., AMH, FSH, AFC) to assess your ovarian reserve and overall fertility health, providing personalized guidance and treatment options.
By proactively addressing these areas, you can empower yourself and significantly optimize your body for conception, answering "What are my chances of getting pregnant at 40?" with a greater sense of preparedness and hope.
What Are the Next Steps if I'm Trying to Get Pregnant at 40?

If you're trying to get pregnant at 40, the most crucial next step is to schedule a comprehensive fertility evaluation with a specialist to understand your unique reproductive health profile. This initial assessment will help clarify your specific challenges and guide you toward the most appropriate and effective path forward, whether that involves lifestyle adjustments, fertility treatments, or exploring alternative options.
Don't wait longer than 6 months of trying to conceive naturally before seeking professional advice, as timely intervention can significantly impact success rates at this age. This proactive approach will provide you with clear answers regarding "What are my chances of getting pregnant at 40?" based on medical facts, not just general statistics.
Actionable Checklist for Your Fertility Journey at 40
Here's a step-by-step guide to navigating your path to pregnancy at 40:
-
Schedule a Pre-Conception Check-up:
- Visit your gynecologist or a fertility specialist for a thorough health review. Discuss your medical history, current health conditions, and any concerns.
- Request essential tests like a full blood count, thyroid function, vitamin D levels, and screenings for STIs.
-
Undergo Fertility Testing:
- For Her: This typically includes blood tests for AMH, FSH, and estradiol (Day 3), and an Antral Follicle Count (AFC) ultrasound to assess ovarian reserve. A hysterosalpingogram (HSG) may also be performed to check if fallopian tubes are open.
- For Him: A semen analysis is crucial to assess sperm count, motility, and morphology.
- Use these results to get a realistic picture of your fertility and inform treatment decisions.
-
Optimize Lifestyle Factors:
- Implement the diet, exercise, and stress reduction strategies discussed earlier. Consider a prenatal vitamin with at least 400 mcg of folate.
- Ensure both partners are committed to healthy habits, as male fertility also plays a significant role.
-
Track Your Ovulation Diligently:
- Consistently use OPKs, BBT tracking, and cervical mucus monitoring to identify your precise fertile window.
- Aim for intercourse every 1-2 days during this window. Tools like a Fertile Window Calculator can assist.
-
Explore Fertility Treatment Options:
- Based on your fertility test results, discuss suitable options with your specialist, such as IUI, IVF (with own eggs or donor eggs), or other assisted reproductive technologies.
- Understand the success rates, costs, and emotional toll of each option.
-
Consider Emotional and Financial Preparedness:
- Fertility treatments can be emotionally demanding and financially significant. Seek counseling or support groups if needed.
- Research insurance coverage and financing options for treatments.
-
Don't Give Up Hope, But Be Realistic:
- While the journey might be challenging, many women successfully conceive and have healthy babies at 40 and beyond.
- Be open to different paths to parenthood, including donor eggs or adoption, if your initial plans don't materialize.
By following these steps, you create a robust framework for your fertility journey, empowering you with knowledge and strategic options as you seek to get pregnant at 40.
Conclusion
Navigating the path to pregnancy at 40 comes with a unique set of considerations, biological realities, and hopeful possibilities. While the natural decline in egg quantity and quality means that conception may require more effort and, often, medical assistance compared to younger years, it is far from an impossible dream. We've explored that your chances of getting pregnant at 40 naturally hover around 5% per cycle, but these odds can significantly improve with the right fertility treatments, particularly IVF, and even more so with donor eggs.
The key takeaway is empowerment through knowledge and proactive action. Understanding your body's fertility status through early testing, optimizing your lifestyle, meticulously tracking your cycle, and most importantly, engaging with a fertility specialist, are paramount. While the journey may present increased risks and challenges, a well-informed and supported approach can lead to a successful and healthy pregnancy. Embrace the process with patience, resilience, and a clear understanding of all the options available to you in 2026.
Actionable Next Steps:
- Schedule a Fertility Consultation: Book an appointment with a reproductive endocrinologist for a thorough assessment of your ovarian reserve and overall fertility health.
- Undergo Comprehensive Testing: Complete all recommended blood tests (AMH, FSH, estradiol) and imaging (AFC, HSG) for yourself, and a semen analysis for your partner.
- Evaluate Treatment Options: Discuss all viable fertility treatment options, including IUI, IVF with your own eggs, or donor egg IVF, based on your test results and personal preferences.
- Optimize Your Lifestyle: Double down on healthy eating, moderate exercise, stress management, and eliminate harmful substances to create the best possible environment for conception.
- Utilize Fertility Tracking Tools: Consistently use an Easy Ovulation Calculator and other methods to pinpoint your fertile window and maximize natural attempts while exploring other options.
FAQ

Is 40 too old to get pregnant?
No, 40 is not too old to get pregnant. While fertility naturally declines with age, many women successfully conceive and have healthy pregnancies at 40 and beyond, often with the help of fertility treatments.
What are the natural chances of getting pregnant at 40 per month?
The natural chances of getting pregnant at 40 per month are generally estimated to be around 5%, decreasing significantly from approximately 20% in a woman's late 20s or early 30s.
How much does IVF cost for a 40-year-old?
The cost of an IVF cycle can range from $15,000 to $30,000 or more per cycle in the U.S., varying by clinic, location, and specific services required (e.g., genetic testing, medication). Costs for women over 40 may be higher due to the potential need for more medication or multiple cycles.
How long should a 40-year-old try to conceive naturally before seeing a doctor?
A 40-year-old woman should consult a fertility specialist after 6 months of consistently trying to conceive naturally without success, due to the accelerated impact of age on fertility.
Is IVF successful at 40 with own eggs?
IVF with a woman's own eggs at age 40 has an estimated live birth rate of approximately 10-15% per cycle, based on data from organizations like SART. Success rates generally decrease after age 42.
What are the risks of pregnancy after 40?
Risks of pregnancy after 40 include higher rates of gestational diabetes, preeclampsia, chromosomal abnormalities in the baby (e.g., Down syndrome), miscarriage, premature birth, and the need for a Cesarean section.
Does a man's age affect fertility when trying to conceive at 40?
Yes, a man's age can also affect fertility. While less dramatic than in women, male fertility can decline after age 40, leading to reduced sperm quality, motility, and a higher risk of genetic abnormalities, which can impact conception and pregnancy outcomes.
What is the success rate of donor egg IVF for women over 40?
The success rate of donor egg IVF for women over 40 is significantly higher than using their own eggs, often reaching 40-50% or more per cycle, as the egg quality comes from a younger, fertile donor.
Can lifestyle changes significantly improve my chances of getting pregnant at 40?
Yes, lifestyle changes such as a healthy diet, moderate exercise, stress reduction, and avoiding smoking and excessive alcohol can significantly improve overall health and optimize the chances of conception at 40, though they cannot reverse age-related egg decline.
References
- American College of Obstetricians and Gynecologists. (2023). Having a Baby After Age 35: ACOG Committee Opinion No. 811.
- Society for Assisted Reproductive Technology (SART). (Accessed 2026). Clinic Success Rates. Retrieved from https://www.sart.org/patients/find-a-clinic/
